Institutional implications for heat related health impacts in the UK
The Climate Change Risk Assessment (Ballard et al., 2012) was commissioned by the UK Department for Environment Food and Rural Affairs (Defra) and published in January 2012. An example socio-institutional network mapping exercise was conducted in the context of a training session for the FP7 Mediation project at the Stockholm Environment Institute in Oxford, UK, using the case below.
The Climate Change Risk Assessment (CCRA)has drawn together evidence and analysis on the risks posed by climate change for the UK. It is being followed up with an Economics of Climate Resilience (ECR) study (Watkiss & Hunt 2011), which will investigate the costs and benefits of adaptation. This study, along with a large number of other inputs, such as from the results of the Adaptation Reporting Powers, will be used to draw up a National Adaptation Programme in 2013.
Work as part of the method development for the ECR study (Watkiss & Hunt 2011) has identified sectoral and cross-sectoral institutional responsibilities and competence for responding to climate risks for heat related mortality and for climate risks on reducing air quality (increasing ozone concentrations, and associated mortality and morbidity). The assessment provided many insights using an institutional analysis of the governance landscape but suggested an enhanced mapping exercise would also be worthwhile.
Background to the risk
One of the primary health concerns (risks) from climate change is heat-related mortality and morbidity. Increased summer temperatures – and heat extremes (heat waves) – currently cause excess heat-related mortality and there is the potential for these to increase significantly in future years with climate change (Defra, 2012). The CCRA highlights that since the excess mortality is associated with higher average daily temperatures as well as with variability and heat extremes, changes in both the average and variability will be important in the future.
The institutional landscape
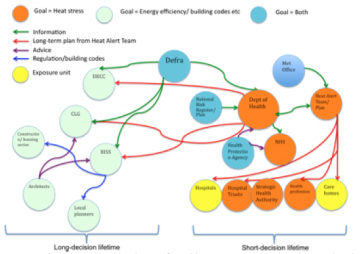
The institutional landscape for heat-related mortality visualised below (elicited through various interviews with an expert) reflects classic redundancies that impede the achievement of the central objective posed here – reduction of mortality under heat stress. Through rich discussions with the expert using this map we were able to identify barriers that are obstacles to achieving the objective, factors that were ‘enabling’ and possible areas for intervention. The main barriers that were identified can be classified in terms of: conflicting goals, ‘thinking in silos’ and different time horizons for decision-making. These are discussed in more detail below.

Image caption: The institutional landscape for addressing a reduction in heat-related mortality based on interviews with the expert. BIS=Department for Business, CLG=Department for Communities and Local Government, Met Office=Meteorological Office, NHS=National Health Service. (The goal of the Met Office is neither of those listed explicitly here – it is simply to provide climate data services in this context).
Based on interviews with the expert.
BIS=Department for Business, CLG=Department for Communities and Local Government, Met Office=Meteorological Office, NHS=National Health Service. (The goal of the Met Office is neither of those listed explicitly here – it is simply to provide climate data services in this context).
The institutional analysis conducted in the CCRA (Ballard et al., 2012, Defra, 2012) and ECR (Watkiss & Hunt 2011) notes that though the main department that has influence and responsibility for heat and health is the Department of Health (biggest circle), there are a large number of cross-government responsibilities, and also a number of inter-related responsibilities regarding public health but also civil emergencies (Defra, 2012). These responsibilities are set out in the Heatwave Plan for England.
The Heatwave Plan for England, which aims to protect health and reduce harm from extreme heat and heatwaves sets out the main responsibility for the public health risks, i.e. what needs to be done by health and social care services and other bodies to raise awareness of the risks relating to severe hot weather and what preparations both individuals and organisations should make to reduce those risks. This also involves the cascade of responsibility down to different governance levels setting out the responsibilities amongst different organisations for different levels of alert (Defra, 2012). The Department of Health is responsible for providing advice and information directly to the public and to health and social care professionals (before a heatwave is forecast and when one is imminent), while the Strategic Health Authority (SHA) must ensure that local services have the capacity and capability to deliver their functions (and to hold the local NHS to account for implementation) and hospitals, care, residential and nursing homes are responsible for monitoring indoor temperatures to reduce the risk of heat related illness and death in the most vulnerable populations (Defra, 2012).
There are also a large number of cross-departmental responsibilities that are relevant to this risk especially in the context of the built environment. The lead department for this sector is the Department for Communities and Local Government (CLG). This has responsibility in relation to building codes and planning. There are also linkages with the Department for Business (BIS) in the building and construction sector and sustainable construction and building standards. The Department for Energy and Climate Change (DECC) also has responsibility for energy use (demand), which is key to the autonomous and planned adaptation response to this risk (air conditioning). Finally, there are policies on spatial policy and planning policy, which involve urban areas and cooling (Defra, 2012). Many of these complex cross-sectoral aspects also cascade down to lower levels of government (e.g. local authorities, local planners) and to the private sector.
Varying time horizons for decision-making
While the main actor responsible for heat-related effects on health is the Department of Health, and there is a Heatwave Plan in place (which was put in place after 2003), this adaptation action does not go far enough to deal with the impacts that may be felt by 2050, which could be more frequent and more prolonged heat-stress events. In addition, some actions by other actors (e.g. improved building codes by BIS) have long-term effects but will only apply to new buildings and infrastructure and not to existing ones, such as hospitals and care homes; the populations of these buildings, the elderly population, are most vulnerable to this stress. This will be compounded by the ageing demographic of the UK population, which will have a higher number of older people (in absolute and relative terms) in future years.
However, as the decision lifetime of the health sector is generally shorter there is less need for long-term capacity building. But non-climatic ‘windows of opportunity’ may need to be exploited in order to address any longer term investments where climate change should be addressed e.g. when building renovations routinely take place (Moser & Ekstrom 2010). This is further complicated by the fact that these buildings (in the health sector in the UK) are often run by private actors (care homes) or in public-private partnerships (hospitals), which makes any government-led initiatives more difficult to implement or enforce through institutions such as the Department of Health or the National Health Service. If a more sophisticated and integrated plan is not put in place, air-conditioning could become a solution for many old buildings, making them both a source of emissions and an exposure unit. E.g. in the case of care and residential homes, and increasing operating costs (from increased energy use).
Conflicting goals
It is clear from the Figure above that the goals of the main actor involved in this issue –the Department of Health – are very different to the goals of the other actors who would need to be involved to deal effectively with this risk. As an example, the other Government Departments have their own strategic objectives that are focused on energy, planning, etc. and not (specifically) health. Long-term adaptation needs to go beyond addressing metrics of relevance for these Departments, which are often currently framed in terms of ‘comfort’, ‘work-productivity’ and energy reduction targets, and this makes a cross-sectoral (and holistic) objective very difficult to achieve. The divergent goals in this landscape and lack of links also mean that there are many opportunities (as visible through this exercise) for intervention and capacity building both structurally in the network and within individual organisations. There could therefore be benefits from more cross-fertilisation of the goals of the different organisations and this could be addressed by creating new types of links, increasing and improving existing ones or by the creation of a new organisation that is designed to facilitate communication between the different actors.
Communication deficit
This lack of common or even overlapping goals further compounds the other issue when looking at the network – that there are only minor links between the Department of Health and these other actors, meaning there is little opportunity to create openings for cohesion or working towards a more harmonised agenda. Defra does have a role in this area through its over-arching ‘Adaptation to Climate Change Programme’ and the oversight of the individual ‘Department Action Plans’ (DAPs) that have been developed, but it is a classical challenge to create ‘joined up thinking’ or an integrated approach to dealing with boundary spanning, cross-sectoral issues. This is not simply a question of ‘finding the answers’ but of organising ways of finding them, agreeing them, trialling new approaches, identifying and dealing with the barriers to change (e.g. those identified in Moser and Ekstrom’s (2010) framework and above all implementing them.
Summary
The institutional landscape for reducing heat related mortality is much more complicated than one might intuitively assume as it includes many other actors whose primary agenda is unrelated to this risk, but who are in fact central to achieving this target long-term. In some ways this might suggest that the climate signal is still too weak or ambiguous for the relevant organisations to act (Berkhout et al. 2006), or that the risk (health) might be low in comparison to the primary focus of other objectives related to energy and buildings. Because stimuli are often not experienced directly by the organisation, Berkhout et al., (2006) suggest that ‘trial-and-error experimentation will not play a significant role in all but extremely climate-sensitive sectors…[….]. In most sectors, organisations are likely to engage in search and assessment processes, suggesting also that the process of adaptation will be managed by higher-level functions in the organisations’ (Berkhout et al., 2006: 152). In this case, this would be the role of Defra and it would seem that this ‘Adaptation to Climate Change’ programme and Department Actions Plans (DAPs) are steps towards at this.
(0) Comments
There is no content